How to Survive Crampy Days. Ways to Reduce Period Pain.
Some people strongly resemble menstrual cramps,
they impart so much pain, but still, without “it”, we panic.
Unknown author

According to Journal of Pain Research, 84.1% of women experience menstrual pain with 43.1% reporting that pain occurs during every period. For the majority of females period cramps are intrinsic to the first days of a woman’s cycle. Yet, is it a norm? In this article, we will discuss what causes menstrual pain, what can alleviate it, and when you should see the doctor.
Is period pain a norm?
Yes, it is. NHS assures us that “Period pain is common and a normal part of your menstrual cycle. Most women get it at some point in their lives.”
In most cases, period cramps (also called dysmenorrhea) are a sign of a healthy body reacting to the shedding of the uterus lining that naturally happens when the egg is not fertilized. Period pain is caused by the muscles in the uterus that contract or tighten. The pain range is vast and can manifest in the following symptoms:
- cramping
- heaviness in the pelvic area
- lower back pain
- stomach pain
- pain in legs
- nausea
- vomiting
- paleness
- diarrhoea
- loose bowels
Cramping is the most common symptom. It can start one or two days prior to menstrual bleeding, and peaks after 24 hours. After that, it may last for two or three days. According to NHS, the pain usually lasts 48 to 72 hours, although it can last longer. As a woman gets older, periods get less painful. Many women also notice an improvement after they’ve had children.
Ways to relieve period cramps
Herbs and spices

Alternative medicine practitioners recommend the following herbs and spices to soothe the period pain:
Five herbal teas
Chamomile tea contains compounds that can help to relieve menstrual cramps and reduce bloating. It happens due to the increase of glycine in your body, the chemical that relieves muscle spasms and acts as a nerve relaxant. Chamomile tea can also stimulate blood flow in the pelvic and uterus, thus regulating irregular periods. The tea is more efficient when you start drinking it a couple of days before your period comes. Hibiscus teacan help relieve menstrual cramps as well as regulate blood pressure, cholesterol level, and digestion. Carnation tearelieves nervousness and nausea, has anti-inflammatory properties and reduces muscle tension in uterine tissues. Rose teahas traditionally been used to reduce PMS symptoms and alleviate menstrual cramps. A randomized controlled trial in Taiwan demonstrated that “drinking rose tea is a safe, readily available, and simple treatment for dysmenorrhea, which female adolescents may take to suit their individual needs”. Black cohosh tea (Baneberry tea) also is known for providing relief for menstrual cramps, menstrual migraines, excessive bleeding, ovarian pain, mood swings, and menopausal hot flashes.
Please, bear in mind that all the herbs mentioned above should be consumed in the recommended amounts. Excessive intake may cause unwanted side effects, such as migraines, headaches, nausea, bleeding, vomiting, and diarrhoea.
Dill
According to a randomized, double-blind study conducted in Iran, dill has shown its effect on the severity of primary dysmenorrhea in comparison with mefenamic acid (a nonsteroidal anti-inflammatory drug used to treat moderate pain). The herb contains compounds that act as antispasmodics (which reduce cramping) and anti-inflammatories (which reduce swelling). Dill seeds can be steeped for 10 minutes and sipped as a tea or added to pickles, salads, soups, and bread.
Turmeric
The plant is traditionally used for thousands of years in Chinese and Ayurveda medicine as an effective natural pain reliever in particular with inflamed pain. Curcumin, the main active component of turmeric, stimulates the body’s natural painkillers and reduces inflammation. This leads to the relief of menstrual cramps. What’s more, a randomized, double-blind, placebo-controlled trial testified to curcumin effectiveness in the alleviation of premenstrual syndrome symptoms.
Fennel
The effect of fennel on pain intensity in primary dysmenorrhoea was proven in a 2012 placebo-controlled trial. Long before the trial, fennel had traditionally been used to relieve painful menstruation. Menstrual cramps are caused by the uterus contracting too intensively. Hence its blood supply is compromised. Fennel works as a muscle relaxant. However, there is one downside – more profuse bleeding.
Cinnamon
Besides the antimicrobial, antibacterial, and antifungal properties, cinnamon can help to regulate blood sugar levels, decrease inflammation and alleviate period pain. This fact was proven by the trial conducted in Ilam University of Medical Sciences, according to which cinnamon is “a safe and effective treatment for dysmenorrhea in young women”.
Ginger
Zingiber (ginger) has traditionally been used to combat the effects of various inflammatory diseases. Ginger contains an enzyme that protects your body from inflammation by inhibiting your body’s prostaglandins production. There’s a direct link between menstrual cramps and the production of prostaglandins because the latter triggers the contractions of the uterus and helps it shed its lining. A randomized, controlled trial featuring 120 residents of Shahed University has proved that ginger has a significant effect on relieving intensity and duration of pain.
Pycnogenol
It is another name for the extract of French maritime pine bark. The plant contains a unique combination of procyanidins, bioflavonoids and organic acids, which offer extensive natural health benefits. The positive effects of pycnogenol on dysmenorrhea were shown in the study published in the International Journal of Women’s Health. Pycnogenol effectively decreased pain scores and the number of bleeding days when administered concomitantly with a low-dose 24/4 oral contraceptive containing gestodene.
CBD

In recent years, CBD has become a buzzword in the wellness industry due to its relaxant and healing properties. CBD (cannabidiol) is a chemical compound found in the plants of the Cannabaceae family that provides a feeling of relaxation and calm. CBD is different from another compound THC in the effect it has on the brain. The former doesn’t get you high. CBD has a similar structure to endocannabinoids found in the body’s Endocannabinoid System (ECS). The ECS’s primary function is to maintain homeostasis within the body and control a range of processes, including pain, memory, mood, appetite, stress, metabolism, sleep, immune and reproductive functions. When a body lacks its cannabinoids, and the ECS becomes dysfunctional, CBD helps to restore homeostasis.
In 2014, PLoS One journal published a study that proves a significant decrease of inflammation and degeneration in those suffering from intervertebral disc disease. Another study conducted in 2016 reports CBD’s positive effects on spasticity—specifically for those with multiple sclerosis.
Since menstrual cramps are a symptom of inflammation and muscle spasms, CBD seems like a promising solution to deal with this issue. At Camilla Organics we have created a CBD tincture that has been specifically formulated for women to use during their periods, Women’s Relief. This is a 15% broad-spectrum CBD oil that works in the ensemble with the traditional herbs Dong Quai, and Wild Yam as well as containing a unique blend of terpenes.
Nutrients

Vitamins B1 and D, Calcium, Magnesium, Zinc, and Omega-3 fatty acids.
Vitamin B1
Vitamin B1 plays an essential role in conducting nerve signals and contracting muscles. Global Journal of Health Science published research on the effects of vitamin B1 on ameliorating the premenstrual syndrome symptoms. B1 is concluded to be effective in the recovery of mental and physical symptoms of PMS. Primary sources of B vitamins are fish oil, green leafy vegetables, cereals, oatmeals and grains, nutritional yeast or vegemite, liver, and mushrooms.
Vitamin D
Vitamin D plays a significant role in calcium balance, bone health, and immune function. In addition to that, it can also reduce the expression of the inflammatory compound cyclooxygenase-2. Thus vitamin D regulates prostaglandin production, exerting anti-inflammatory effects in the body and endometrium. A randomized, double-blind placebo-controlled clinical trial confirmed the effectiveness of vitamin D in primary dysmenorrhea treatment. Primary vitamin D sources include sunshine, fatty fish, foods fortified with vitamin D (e.g., dairy products, orange juice, soy milk, and cereals), beef liver, egg yolks.
Calcium
Calcium supports our bones and muscles, and its deficiency poses a serious health risk for women. A double-blind, randomized clinical trial published in Nutrients Journal concluded that treatment with calcium supplements is an effective method for reducing mood disorders during PMS. Primary sources of calcium include milk, dairy foods, green leafy vegetables (except spinach), soy products, nuts, bread and anything made with fortified flour, fish where you eat the bones (e.g., sardines and pilchards).
Magnesium
Magnesium normalizes the actions of different hormones (mainly progesterone) on the central nervous system. Magnesium works best in combination with vitamin B6, which is proven by the research published in the Iranian Journal of Nursing and Midwifery Research. Vitamin B6 and Magnesium significantly decrease PMS. Primary sources of magnesium are green leafy vegetables, fruit, nuts and seeds, legumes, peas, baked beans, seafood, whole grains, raw cacao, dark chocolate, tofu, chlorella powder.
Zinc
Zinc has been found to relieve menstrual cramps and swelling since it exerts antioxidant and anti-inflammatory effects in the uterus. Oman Medical Journal has published research on the efficacy of zinc administration in the treatment of primary dysmenorrhea. It runs “The use of a zinc supplement in combination with mefenamic acid was superior in reducing primary dysmenorrhea compared to mefenamic acid alone.” Primary sources of zinc are meat, shellfish, legumes, seeds, nuts, dairy, dairy, eggs, whole grains, and dark chocolate.
Omega-3 fatty acids
International Journal of Gynecology & Obstetrics published research confirming that supplementation with omega-3 fatty acids reduces the symptom intensity of primary dysmenorrhea. However, be careful with the supplement. Omega-3 fatty acids may provoke intensive bleeding, especially if a woman takes blood thinners such as clopidogrel (Plavix), warfarin (Coumadin), or aspirin. Please, consult your doctor before taking the supplement additionally. Natural sources of omega-3 fatty acids include salmon, herring, cod liver oil, oysters, sardines, anchovies, caviar, flax seeds, chia seeds, walnuts, and soybeans.
Heat

Applying heat (heating pad, heat wrap, hot water bottle or warm towel) to your abdomen and lower back is a quick way to relieve menstrual pain. A study published in BMC Women’s Health has proved that a heat patch is as effective as ibuprofen. A warm bath and shower is also a great pain soother since it relaxes tense muscles.
Exercise

Exercise releases endorphins, brain chemicals that promote general well-being and can help women to combat period pain.
- Journal of Women’s Health published research suggesting that aerobic activity may be the best combatant to painful menstrual cramps. This activity increases blood flow and releases beta-endorphins which relieve pain.
- The following yoga poses focus on opening the hips and relaxing the pelvis: seated spinal twist, supine hip opener and child’s pose.
- Light weight lifting also increases blood flow to the muscles and helps alleviate pain associated with your menstrual cycle. Try sumo squat, medicine ball chop and medicine ball slam. However, don’t do any of these exercises if you have a heavy flow.
Massage

Iranian Journal of Nursing and Midwifery Research published research concluding that massage therapy can be a fitting method to reduce the menstrual pain caused by endometriosis. Massaging your abdomen for as little as 5 minutes a day encourages blood flow in this area and may be able to help relieve menstrual cramps.
Acupuncture and Acupressure
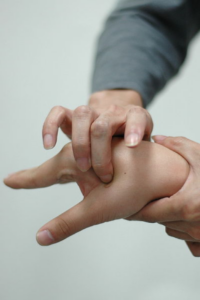
These eastern healing treatments can stimulate specific trigger points (on the back, abdomen, feet, and the fleshy part between your thumb and index finger) on the skin which produce desired effects in the body. Medicine (Baltimore) journal published research suggesting that acupuncture might be used as an effective and safe treatment for females with primary dysmenorrhea.
When it’s time to see a doctor

Severe menstrual cramps may be a symptom of an underlying medical condition. If you feel that period pain prevents you from normal functioning, you begin to get severe cramps after the age of 25 years or you resort to painkillers at the beginning of every cycle, it’s time to visit your gynaecologist. The list of conditions behind painful periods includes Endometriosis, Fibroids, Pelvic inflammatory disease (PID), Polycystic ovary syndrome (PCOS), Cervical stenosis, and Adenomyosis, to name a few.
Apart from reviewing your medical history, your doctor will perform a physical exam and may also give you a pap test (a screening procedure for cervical cancer). Additional tests might include an ultrasound to check, a CT scan, and gynecologic laparoscopy.
https://www.ncbi.nlm.nih.gov/pmc/articles/PMC3392715/
https://www.womens-health-concern.org/help-and-advice/factsheets/period-pain/
https://www.yourquote.in/tags/cramps/quotes
https://www.naturalcycles.com/cyclematters/what-causes-period-cramps/
https://www.healthline.com/health/severe-menstrual-cramps
https://flo.health/menstrual-cycle/health/period/tips-to-reduce-period-cramps
https://www.nутмшhs.uk/conditions/period-pain/
https://www.healthpartners.com/blog/when-to-see-a-doctor-for-menstrual-cramps/
https://www.webmd.com/women/ss/slideshow-get-rid-of-cramps
https://www.abetterflorist.com/blog/5-flower-teas-beneficial-period/
https://www.ncbi.nlm.nih.gov/pubmed/16154059
https://www.ncbi.nlm.nih.gov/pmc/articles/PMC4115348/
https://www.webmd.com/drugs/2/drug-11586/mefenamic-acid-oral/details
https://www.ncbi.nlm.nih.gov/pubmed/26051565
https://goldengrind.com.au/blogs/news/turmeric-helping-with-period-pain-or-endometriosis
https://www.ncbi.nlm.nih.gov/pmc/articles/PMC3611645/
https://nutritionfacts.org/2018/07/19/fennel-seeds-vs-ginger-for-menstrual-cramps-and-pms/
https://www.ncbi.nlm.nih.gov/pmc/articles/PMC4443385/
https://www.avogel.co.uk/health/periods/can-cinnamon-help-period-cramps/
https://www.ncbi.nlm.nih.gov/pmc/articles/PMC3518208/
https://www.period.media/spotlight/how-drinking-ginger-can-help-against-menstrual-cramps/
https://www.eurekalert.org/pub_releases/2008-06/mg-nsp061808.php
https://alphagreen.io/women-s-relief-tincture-10ml.html
https://www.remedyreview.com/health/can-cbd-help-reduce-period-pain-and-menstrual-cramps/
https://www.ncbi.nlm.nih.gov/pmc/articles/PMC4269422/
https://www.ncbi.nlm.nih.gov/pmc/articles/PMC4710104/
https://www.delune.co/blogs/blog/vitamin-b1-period-cramps-naturally
https://www.ncbi.nlm.nih.gov/pmc/articles/PMC4825494/
https://www.ncbi.nlm.nih.gov/pmc/articles/PMC6265788/
https://www.talltreehealth.ca/blog/2017/3/29/vitamin-d-and-menstrual-cramps
https://www.ncbi.nlm.nih.gov/pmc/articles/PMC5313351/
https://takecareof.com/articles/best-supplements-pms-symptoms
https://www.ncbi.nlm.nih.gov/pmc/articles/PMC3208934/
https://www.huffingtonpost.com.au/2017/07/10/what-foods-contain-magnesium_a_23024245/
https://www.ncbi.nlm.nih.gov/pmc/articles/PMC4861396/
https://www.ncbi.nlm.nih.gov/pubmed/17289285
https://www.ncbi.nlm.nih.gov/pubmed/22261128
https://www.ncbi.nlm.nih.gov/pmc/articles/PMC6214933/
https://bmcwomenshealth.biomedcentral.com/articles/10.1186/1472-6874-12-25
https://www.huffpost.com/entry/3-types-of-exercise-prove_b_11318472
